Updated/reviewed by the authors, July 2017.
Surgery in AMD
Authors:
Angelina Meireles, MD
Hospital Santo António-CHP - Porto, Portugal
Bernardete Pessoa, MD
Hospital Santo António-CHP - Porto, Portugal
Natália Ferreira, MD
Hospital Santo António-CHP - Porto, Portugal
Rui Martinho, MD
Hospital Lusíadas Porto - Porto, Portugal
Introduction
In recent years, new treatment modalities such as photodynamic therapy and intravitreal anti-VEGF injections have been added to the treatment armamentarium for age-related macular degeneration (AMD).
Prior to the introduction of these therapies, only laser photocoagulation had been shown in a large randomized controlled trial to confer a statistically significant benefit in the treatment of subfoveal choroidal neovascularization (CNV) secondary to AMD regarding to long-term visual acuity when compared to the natural history of the condition(1-3).
Unfortunately, the Macular Photocoagulation Study also showed that laser photocoagulation was associated with immediate average reduction of visual acuity, with benefits over no treatment apparent only six months after treatment(1-3).
In fact, recovery of good vision rarely occurred in these patients.
As a result of the limited treatment options, alternative therapies, such as submacular surgery for CNV removal, were pursued with limited or no success.
Meanwhile, a different management paradigm for AMD was established with macular translocation.
However, because of its higher risk of complications, its popularity has waned with the wider availability of photodynamic therapy and the introduction of intravitreal anti-VEGF agents.
Nonetheless, they remain potentially useful treatment options, even if their role in the management of AMD is neither established nor consensual.
In the meantime, vitreoretinal surgery and vitrectomy have had important developments, mostly due to advances in sutureless transconjunctival vitrectomy, use of dyes, tamponade agents and new equipments.
Novel surgical approaches for AMD are under scrutiny: the association of submacular surgery with pigment cell transplantation, the use of adjuncts, such as recombinant tissue plasminogen activator (r-TPA) for subretinal hemorrhages displacement combined with anti-VEGF treatment.
Recently, a new insight involving the vitreoretinal surface has been proposed for the pathophysiologic mechanisms underlying the development of CNV in AMD.
Accordingly, posterior vitreomacular adhesion may be another risk factor in a subpopulation of patients with wet AMD, opening another path for a surgical approach in the treatment algorithm for this condition(4-7).
Future studies are needed to define the role of vitreoretinal surgery in such cases.
Macular translocation
The first experiments on retinal relocation were conducted and reported in the beginning of the 80’s.
Their aim was to study the anatomic dependency of the foveal retina on foveal retinal pigment epithelium (RPE) and choroid.
The assumption that visual function could be preserved with foveal displacement has originated from cases of ectopic macula from retinal traction or after surgery in patients with retinopathy of prematurity and retinal detachments with giant tears(8).
They ended up showing the feasibility of rotating the macula around the optic disc with reattachment of the fovea in animal eyes(9).
One might say that this was the starting point for the idea of rotating the macula of eyes with subfoveal CNV to a new area of underlying RPE-Bruch’s membrane-choriocapillaris complex – macular translocation – as a treatment for the condition.
Although the exact pathogenesis of CNV secondary to AMD is not known, the natural history of this condition is a progressive loss of central vision over time.
The initial retinal dysfunction responsible for impaired vision in eyes with subfoveal CNV may be attributable to factors such as subretinal fluid, subretinal hemorrhage and retinal edema.
When fibrous proliferation and degeneration of the overlying photoreceptors occur during the later stages of the disease, the visual loss becomes irreversible.
The rationale of macular translocation is that moving the neurosensory retina of the fovea in one eye with recent-onset subfoveal CNV to a new location before the occurrence of permanent retinal damage, may allow it to recover or to maintain its visual function over a healthier bed of RPE-Bruch’s membrane-choriocapillaris complex.
In addition, relocating the fovea to an area outside the CNV allows the ablation of the later, by laser photocoagulation without destroying the fovea, in an attempt to preserve central vision.
On the other hand, some surgeons have combined macular translocation with CNV removal, allowing the fovea to be relocated to an area outside the RPE defect created during submacular surgery.
Several different surgical techniques for macular translocation have been described and were currently used.
These techniques produce different degrees of postoperative foveal displacement, and can broadly be classified into two categories:
Full macular translocation, and limited macular translocation.
Full macular translocation
After developing their surgical techniques in rabbit eyes(9), Machemer and Steinhorst became, in 1993, the first surgeons to demonstrate the feasibility of macular translocation in humans(10,11).
Their technique involved lensectomy, complete vitrectomy, planned total retinal detachment by transretinal infusion of fluid under the retina, 360º peripheral circumferential retinotomy, rotation of the retina around the optic disc, and reattachment of the retina with silicone oil tamponade.
Besides allowing retinal rotation to occur, the retinotomy also made way to the subretinal space for syncronous blood and CNV removal.
Since then, a number of investigators have subsequently modified this technique(12-15).
Corrective extraocular muscle surgery for globe counter-rotation, due to frequent postoperative cyclovertical diplopia or awareness of a tilted image, may be done during the primary surgery or at a later stage(13,16).
While some surgeons have found the results of macular translocation encouraging(13,17-20), others found the surgery unpredictable(21,22).
In a series of 50 consecutive eyes with subfoveal CNV from AMD that underwent full macular translocation followed-up for a median period of 21 months (12-36 months), Pertile and Claes reported an improvement of ≥ 2 Snellen lines in 66%, while 28% remained stable (±1 line) and 6% decreased by ≥ 2 lines(17).
Van Romunde et al. published long-term results of full macular translocation, in a retrospective study, of 158 patients with subfoveal CNV from AMD followed-up for a mean period of 45 months (12-108 months). A clinically and statistically significant improvement of best-corrected visual acuity (BCVA) was detected and sustained for up to 5 years after full macular translocation. They found that 45% had a 3-line or more gain at last visit. In a subgroup of 56 patients followed up for 5 years or more, there was a gain of 1.5 lines compared with preoperative BCVA(19).
In a series of 40 consecutive patients with subfoveal CNV from AMD, who undergone the mentioned surgical technique and with a mean follow-up period of 37.6 months (12.4-67.4 months), Chen et al. reported at the last observation that 68% achieved a BCVA of 6/60 or better, 43% achieved 6/30 and 15% 6/12 or better. A 3-line gain in BCVA was obtained in 30% at 1 year and in 25% at the most recent follow-up. However, in 25% of patients achieving 6/60 or better at 1 year, BCVA declined by greater than 2 lines primarily as a result of recurrent CNV(20). In another prospective, interventional, consecutive non-comparative case series of 61 AMD patients who underwent the same procedure and followed-up for 12 months, the visual acuity improved by ≥ 1 Snellen lines in 52%(23).
Toth et al. also showed improvements in distance and near visual acuity, contrast sensitivity and reading speed in a series of 25 consecutive AMD patientss(24).
In addition to exceptional surgical technique, avoiding intra and postoperative complications, the key for success after macular translocation seems to be patient selection(25,26).
If this procedure is performed on a patient without viable foveal photoreceptors, there is no chance for visual improvement.
Still, the main drawback of macular translocation lies on its high rate of complications. Rhegmatogenous retinal detachment, with or without proliferative vitreoretinopathy development, is the most common serious complication of macular translocation. Rates up to 19% have been reported(27).
Persistent or recurrent subfoveal CNV has been described in up to 30% of patients undergoing this procedure(19,27). Almost all reported cases of recurrent CNV occurred at the edge of the RPE defect created by the CNV excision. In order to reduce the recurrence of CNV, the fovea needs to be reconstructed by using healthier RPE such as those derived from stem cells (28). Chen et al. recommend close monitoring of the edge of excision site, clinically and with SD-OCT, to detect early signs of CNV. Prompt initiation of a course of anti-VEGF therapy can maintain visual acuity gained following translocation(20).With a longer follow-up, cystoid macular edema (CME) and subfoveal RPE atrophy may be limiting factors for improved postoperative visual acuity. Terasaki and colleagues found a 70% incidence rate of CME(29). Chen et al. described CME in 38 of patients (95%), at some stage postoperatively(20).
In a long-term follow-up, Aisenbrey et al. (14 to 79 months – mean 38) and von Romunde et al. (12 to 108 months – mean 45) reported 28% versus 47% of patients with subfoveal atrophy by the third and fifth year postoperatively respectively(18,19).
In figures 1 and 2, we present two anecdotal cases in which full macular translocation was performed. They presented with extensive submacular hemorrhages that were considered inadequate for anti-VEGF therapy. Visual rehabilitation was achieved, enabling the patient’s independence for daily activities.
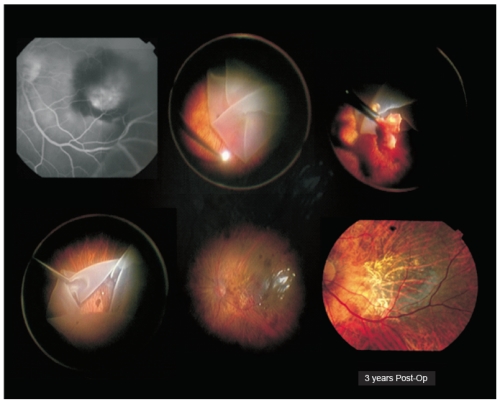
Figure 1. Case I – Patient with severe visual acuity loss in his left eye 3 days before admission (right eye was lost to advanced AMD). He presented with a submacular hemorrhage complicating wet AMD. Full macular translocation was performed (António Travassos – Coimbra Surgical Centre, Coimbra, Portugal). Three years after surgery, left eye visual acuity was 20/200.
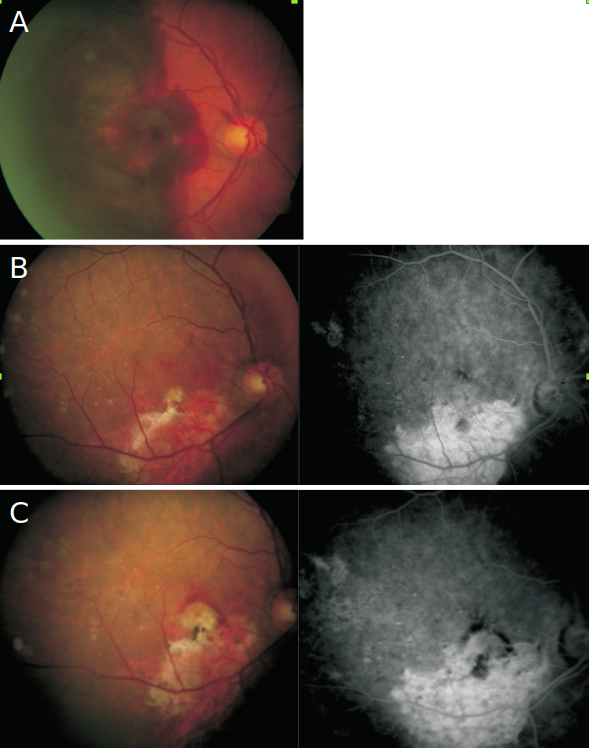
Figure 2. Case II – A 85-year-old man with an extensive submacular hemorrhage associated with subfoveal CNV (A). Four months after a full macular translocation (Claus Eckardt-Staedtische Kliniken Frankfurt A.M., Germany) his visual acuity was 20/80 (B). A recurrent subfoveal CNV developed after the first year of follow-up, and the patient was started with intravitreal ranibizumab injections. After 4 treatments, a visual acuity of 20/63 remained stable (C).
Limited macular translocation
In an effort to overcome the major complication following macular translocation with large retinotomy, proliferative vitreoretinopathy, de Juan developed a new technique in 1998(30).
His technique involved transretinal hydrodissection using small posterior retinotomies to induce a subtotal retinal detachment, a complete vitrectomy, anterior-posterior shortening near the equator and retinal reattachment.
As no large retinal break was created, the likelihood of developing proliferative vitreoretinopathy was thought to be lower.
As more experience was gained with this surgery, additional modifications were made to the original technique.
This is essentially a five-step procedure. It starts with the placement of scleral imbricating sutures (either in the superotemporal or inferotemporal quadrants for inferior and superior translocations, respectively) for antero-posterior shortening of the eyewall, followed by a pars plana vitrectomy with posterior vitreous detachment induction.
The third step should be an internal subretinal hydrodissection through small self-sealing retinotomies for creation of a partial neurosensory retinal detachment.
After tightening the scleral imbricating sutures, a redundancy of the neurosensory retina relative to the eyewall is created that should allow the desired foveal displacement, after retinal reattachment with fluid-air exchange.
Limited macular translocation may be either inferior or superior, depending on the movement of the neurosensory macula relative to the underlying tissues.
The largest series of limited macular translocation by Pieramici et al., in a retrospective review, analysed the outcome of 102 consecutive eyes of 101 patients that underwent inferior limited macular translocation for AMD-related subfoveal CNV. At three and six months postoperatively, 37% and 48% of the eyes, respectively, experienced ≥ 2 Snellen lines of visual improvement(31).
After one year of follow-up, 39.5% still maintained a ≥ 2 lines of improvement, while 29.0% remained unchanged and 31.4% lost ≥ 2 lines of visual acuity(32).
Recurrent CNV developed in 34.6% of the eyes, being subfoveal in most of the cases (65%)(32).
Besides the usual risks inherent to pars plana vitrectomy, limited macular translocation is associated with additional risks similar to those of scleral buckling surgery.
As with full macular translocation, the rate of complications won its popularity.
Although conceived in an effort to reduce the rate of proliferative vitreoretinopathy development, this has remained the most common serious complication after limited macular translocation.
Rates of retinal detachment up to 17.4% have been reported(33).
Insufficient macular translocation is another important limitation of this procedure, restricting its indications to smaller CNV.
Is there a role for macular translocation in the current era of anti-VEGF therapy and combined treatments?
IIn the latest edition of Vitreous Microsurgery (5th Edition, 2011 - Lippincott Williams & Wilkins)22),
Steve Charles et al. stated again that do not believe that this procedure is indicated due to the high incidence of complications.
In the review from Eandi et al. to access the functional outcomes of macular translocation for wet-AMD was concluded that there wasn’t enough evidence in randomized trials to support the benefit of surgery(34).
Future studies should involve patients with small neovascular membranes that are non-responsive to the present medical armamentarium, and that accept the risks of surgery in an effort to improve their visual function.
This is a procedure that demands a high level of surgical skill and experience, with a rather flat learning curve. The number of complications is unacceptably high. The widely use and quite effective pharmacologic therapy has limited this surgical modality to patients with large submacular haemorrhages, or patients unresponsive to VEGF inhibitors(19).
At the present time, the very small incidence of cases that could benefit from this procedure does not allow every Ophthalmology department with vitreoretinal surgical capability to gain expertise on macular translocation.
Referral this few cases to selected surgical units with the proper human and technical resources and experience seems the best choice.
Submacular surgery
As already has been said, a variety of surgical treatments have been developed for exudative AMD disease and one of those are the different modalities of submacular surgery.
We will review these surgical approaches and their actual role in the AMD treatment.
Surgery with subfoveal neovascular membrane removal
In 1988, Juan and Machemer(35)
published the first results of vitreous surgical techniques on removal of blood or fibrous submacular complications in four AMD patients.
Countless publications of retrospective small sample size studies ensued, with no control group, describing the benefits of this technique in stabilizing the disease, albeit displaying reduced functional benefits(36-38).
The need to establish the benefits of submacular surgery in the treatment of CNV led to the Submacular Surgery Trials (SSTs). One of the aims of this study was to find out if surgery, for the different types of AMD lesions, more than vision stabilization, was able to increase vision with real impact in the life quality of these patients(39).
The pilot trial used to pre-test the research procedures of this multicentre, randomized, controlled study found no reason to prefer submacular surgery to laser photocoagulation in AMD patients with similar lesions to those displayed by study patients(40).
Several surgical techniques are described in the literature. In summary, these techniques include standard pars plana vitrectomy, with or without posterior hyaloid membrane removal; posterior retinotomy followed by infusion of subretinal saline solution or r-TPA into lesions with a large haemorrhagic component, membrane mobilization and its removal with surgical forceps, followed by eventual aspiration of fresh blood or clot, depending on the situation.
Possible intraocular haemorrhages during surgery may be controlled by increasing the intraocular pressure, either by raising the infusion bottle or using heavy perfluorocarbon liquids.
The procedure is finished with a fluid-air exchange, followed by gas buffering, maintaining the patient in the prone position until gas reabsorption(41-44).
Due to the physiopathology of this disease, it was observed in histopathological studies that inadvertent and undesired removal of the pigment epithelium often occurs during membrane removal, especially for type 1 membranes.
The irreversible absence of the pigment epithelium leads to loss or atrophy of photoreceptors and choriocapillaries, inducing an unfavourable visual recovery(45).
The percentage of removed epithelium is variable but may reach significantly high values, as observed in the SSTs, where the pigment epithelium was involved in 84% of removed membranes(46). ther complications like regmatogeneous retinal detachment were also observed, with higher incidence in eyes with larger hemorrhagic lesions and relatively poor visual acuity(47).
Therefore, both the functional results and the impact on life quality observed for the various subgroups considered in the SSTs, compared to natural disease progression, led the authors not to recommend submacular surgery as a treatment option(48-51).
Retinal pigment epithelium transplants
As previously referred, the poor results achieved with surgical removal of subfoveal membranes, largely due to resulting atrophy or rupture of the photoreceptor-RPE complex, led some groups to combine neovascular membrane removal with simultaneous autologous transplant of iris or RPE, in order to restore normal subretinal conditions(52-54).
The surgical maneuvers were similar to those used for subfoveal CNV removal with additional aspiration and subsequent pigment epithelial cell transplant procedures.
Although good tolerability has been demonstrated for pigment cells in the subretinal space, as well as absence of membrane recurrence, the poor functional results obtained in most studies have been attributed to several factors, including lack of differentiation in pigment cell reproliferation, failure in adhesion to Bruch’s membrane and failure to form a regular pigment epithelial cell monolayer(52-56).
Also according to other authors, the behavior of transplanted cells depends essentially on the type of environment found at the seeding location(57).
Meanwhile, Peyman et al. described a technique in which an autologous pedicle graft or homologous RPE cells and Bruch’s membrane replaced the submacular RPE(58). At mid-90s, Algvere et al. transplanted fetal RPE as a monolayer patch or in a suspension form(59,60).
LLater on, Aylward et al., from Moorfields Eye Hospital, were the first team to describe the concept of total patch translocation of the RPE-choroid complex to the subfoveal area(61). The patches collected in the macular area near the RPE lesion were small and even so they survived in the subfoveal space (assessed by OCT, FA and ICG angiography); after 5 years of follow-up, none of the nine transplanted patients displayed any function, what might be explained by chronic photoreceptor apoptosis(62).
In Rotterdam, Van Meurs et al., described a modification to this technique in which a healthier full-thickness patch of RPE-choroid of approximately 1.5x2 mm is harvested from within a circular zone isolated by heavy diathermia in the superior midperiphery where cells were thought to be less damaged(63). he group reported long-term results (up to 7 years) of at least 20/200 final BCVA in 15% of patients and the main complications were recurrence of CNV (10%) and proliferative vitreoretinopathy (10%)(64).
Subsequently, other groups have been publishing small case series presenting not only expressive and sustained improvement in visual acuity and reading ability, but also recovery of central fixation, evidence for grafts revascularization (also demonstrated histologically in animals experiments) and a normal autofluorescence over the patch in patients with exudative or dry AMD(63-72).
According to Parolini et al., those eyes whose vision is not seriously impaired (equal or higher than 20/200) and with a relatively well-preserved retinal layers, especially the external limiting membrane, are the ones with better outcomes. In this series, long-lasting beneficial effect of the graft for the function of the retina with improvement of vision was observed in most cases(73). Another critical issue for a successful outcome is the blood supply to the graft. Cereda et al. reported partial revascularization of the patch with choroidal vessels running parallel to one another unlike the radially choroidal vascular system in the macula area. In some cases localized feeder vessels, usually at the graft margin, were seen. These vessels are probably a large choroidal artery arising from the connection between the patch and the original choroid or choriocapillaris(74,75).
During CNV removal, choroidal structure should be left unharmed and the dimension of the graft must be large enough to connect to an area of preserved choroid. Revascularisation is a progressive event and time to completion is variable (over 1 month). Before revascularisation, patch survival may be accomplished through plasmatic diffusion, as in skin transplantation(76).
RPE-choroid transplant offers an interesting alternative to macular translocation, especially in patients with good vision in their fellow eye. This surgery is challenging and not free from intraoperative and postoperative complications. Improvements in microsurgical techniques can lead to less traumatic CNV removal and insertion of the RPE-choroid graft. This is crucial for promising functional results, as well as an adequate patient selection.
Management of submacular haemorrhage
In addition to the poor prognosis, exudative forms of AMD evolved into a major submacular haemorrhage that are difficult to diagnose (concerning membrane location and extension) and to treat(77,78).
n the era of antiangiogenic agents, this is the most frequent form of AMD for which surgery is indicated, aiming to avoid further blood damages (mechanical, metabolic and toxic) to the photoreceptor-RPE complex(41,79,80).
As previously referred, blood was initially removed by aspiration or mechanically extracted.
In 1991, Lewis et al. were the first researchers to report the fibrinolysis properties of r-TPA, which made this agent useful in removing blood clots(42-44,81-84).
In order to avoid surgical manipulation of the macular retina, Herriot described a procedure involving displacement of submacular blood by intravitreal injection of r-TPA and gas, followed by prone position, for the first time in 1997.(84)
Blood is normally displaced temporally or infero-temporally, with a significant increase in visual acuity occurring immediately after the aforementioned procedure, as described in countless published outcomes.
Some authors have pointed out the duration of hemorrhage (the shorter the better) as the main predictive factor for the aforementioned improvement(85-92).
On the other hand, the usefulness of intravitreal r-TPA as an adjuvant to this technique has been questioned, not only because r-TPA diffusion to the subretinal space has not been proved in experimental studies, but also because some studies demonstrated the success of pneumatic displacement of subretinal blood without concomitant injection of r-TPA(90,91,93).
Therefore, Haupert introduced a hybrid technique in 2001, combining the concepts of pneumatic displacement with subretinal r-Tpa(94).
After a few changes, this technique is currently used in some centers, as described: pars plana vitrectomy, removal of the posterior hyaloid, injection of r-TPA (12.5 or 25 μg/0.1 mL) into the subretinal clot using a 39 or 41-gauge flexible translocation cannula and fluid-air exchange followed by prone position(95).
The advantages of this technique over the surgical blood removal are less intra and post-operative complications, which is probably due to the smaller extent of tissue manipulation and consequent reduction in retinal injury(83,94,95). Usually after successful blood displacement, the patient experience a short gain in visual acuity that frequently drop down because of recurrent and massive haemorrhage or progression of the underlying disease. Such cases might benefit from more invasive procedures as vitrectomy and 180º retinectomy for direct access to subretinal space allowing the complete removal of the underlying blood and CNV(96,97).
Since the advent of anti-VEGF therapy, a combined intraocular injection of bevacizumab and r-TPA seems to be a promising treatment for AMD with submacular haemorrhage. Whatever the chosen procedure, close observation and additional intra- and/or postoperative anti-VEGF treatments might potentially prevent CNV related complications(98-100). n selected cases, namely patients with multiple diseases and little subretinal blood, monotherapy with intravitreal anti-VEGF could offer some chance of visual improvement with a minimally invasive approach(101).
More recently, there has been a trend towards more complex associated procedures: vitrectomy and gas endotamponade with subretinal injection of r-TPA and anti-VEGF agents (1.25 mg bevacizumab). The thinking is that vitrectomy may relieve any vitreomacular traction, preventing wet-AMD from getting worse. Regarding subretinal anti-VEGF application, it ensures the direct delivery of the drug at the site of the CNV, which may enhance its effect; the short half-life of r-TPA (around 5 minutes) may reduce the risk of drugs interaction when given alongside anti-VEGF agents, particularly when injected into the confined subretinal space(98,102-104). In 2013, Martel et al. advocated a combined subretinal injection of r-TPA, bevacizumab and filtered air (0,2 mL), followed by intravitreal fluid-air or hexafluoride gas exchange and up-right positioning in order to get an easier hemorrhage displacement due to the lowering haemorrhage’s buoyancy obtained by the subretinal air(105).
As occurs in other macular diseases and also previous referred, the detection on OCT of an ellipsoid layer and external limiting membrane line beneath the fovea are strongly correlated with good visual prognosis(106). A study that used SD-OCT to evaluate the preoperative features of submacular haemorrhage and PED in nAMD, found out that the presence of an intact ellipsoid layer and lower height of submacular haemorrhage were predictors of good postoperative BCVA. In contrast, the preoperative characteristics of PED had no effects on visual prognosis(107). In the recent Stanesc-Segall literature review the greatest improvement is obtained when a combined approach with vitrectomy, subretinal r-TPA, intravitreal gas and anti-VEGF is performed(104). However, according to others, subretinal r-TPA, intravitreal gas and anti-VEGF treatment without vitrectomy, which is a less invasive procedure, had also good functional results with acceptable safety and fewer complications(100).
Concomitant systemic anticoagulation or platelet anti-aggregant medication should be discontinued if possible, especially in monocular patients. With the improvement of vitreoretinal surgery and instrumentation, described techniques are reasonably effective, although with widely variable outcome, depending on the severity of the underlying disease. Post-surgical addition of anti-VEGF medications appears to help preserve vision over time.
Regardless treatment modality, the benefits of surgery diminish with an increasing duration, extension and thickness of submacular haemorrhage(108).
Submacular haemorrhage associated with CNV due to AMD is a potentially visually devastating condition and to date, there is no consensus regarding an optimal treatment.